
As we celebrate National Nurses Week from May 6th to 12th, let’s reflect on how we can empower the untold heroes of hospitals to deliver excellent patient care. On the frontlines every day, as Dr. William Osler, the founder of Johns Hopkins University aptly summarized it, “the trained nurse has become one of the great blessings of humanity, taking a place beside the physician…” Despite the key role they play, more needs to be done to empower them to do the best work they can.
Nurse Educator and Author Sharon Hudacek hit the nail on the head, highlighting how “bound by paperwork, short on hands, sleep and energy… nurses are rarely short on caring.” The main touchpoint between patients, their loved ones and the medical system, too often nurses are compelled to step away from caring, supporting and helping patients to fill out forms and file reports.
In too many hospitals, nurses spend hours away from patients manually completing reports chasing down colleagues for information and tackling reams of past paperwork whenever information is needed. Outdated and antiquated systems like this do a disservice to the noble profession of nursing, to hospitals and ultimately to patients.
At Prista Corp., we know there’s a better way.
Nurses need a system that allows them to quickly and easily report on incidents, a system that allows seamless collaboration across the hospital, and most importantly, a system that allows everyone to use data to drive their decision-making. It’s this vision of an innovative, collaborative system that minimizes busy work that motivates our team of experienced clinical professionals when developing and optimizing ActionCue.
Ahead of her 204th birthday, we hope to continue embracing Florence Nightingale’s advice that we must “never consider ourselves finished, nurses. We must be learning all our lives.”
This article first appeared in the May 2024 edition of Marketplace, the monthly newsletter of TORCH Management Services, Inc.

Patient Safety is defined as “the absence of preventable harm to a patient and reduction of risk of unnecessary harm associated with health care to an acceptable minimum.” Every hospital in America has a stated mission to prioritize Patient Safety above all else. “First, do no harm” is the most fundamental principle of any health care service. Every healthcare organization says it, but are they really doing everything they can to prioritize patient safety?
The first step to solving a problem is admitting that you have one. But what if you aren’t aware that you have a problem? Especially in the Critical Access and Community Hospital space, where staff is stretched to non-optimal lengths, how can a facility, not only stay on top of patient safety, but take the time necessary to rigorously evaluate processes and policies to improve their quality of care?
Beyond the moral and ethical obligation to provide the best health care possible, there are clear financial benefits, although often unrecognized, unknown, or undervalued, to doing no harm. When was the last time you truly evaluated your facilities process of minimizing risk events, and optimizing quality outcomes? Could it be improved upon? Can it make your facility more profitable? The answer is a resounding yes.
Look at your patient fall data to see how much you’ve paid for Cost of Harm falls last year – what else could your hospital have used that money for? Next time you need to tighten your budget, remember cost cuts don’t just come from lowering staffing or standards. You can also save by minimizing how much quality and risk incidents are costing your hospital.
We’ve found this is true amongst our customers. Using ActionCue© CI’s Performance Improvement Plans and the guidance of our Implementation & Support team, one of our customer hospitals reduced falls at their facility by 25% over three years. Based on the Center of Disease Dynamic’s Cost of Harm figures, this saved them almost a million dollars in additional costs.
Another hospital saved more than a million dollars over three years as their CLASBI cases reduced by almost 47%. A third hospital saved more than $80,000 by cutting their rate of VAP cases by 66% in three years of using ActionCue CI.
Improving the quality of care, through proactively tracking and tackling risk and quality incidents can lead to significant savings from the cost of harm avoided – money that can fund additional staff, equipment upgrades and other improvements.
This positive cycle can multiply – every dollar saved by avoiding a Cost of Harm event can be spent on further eliminating Cost of Harm events, leading to more savings from the cost of harm avoided. As the cycle continues, avoidable costs decrease while the quality of care – and your reputation – increases.
This article first appeared in the March 2024 edition of Marketplace, the monthly newsletter of TORCH Management Services, Inc.

Prista's Founders, Don Jarrell and Billie Anne Schoppman were interviewed recently by Michelle Shaffer, Director of Business/Program Development at the Center for Improvement in Healthcare Quality (CIHQ).
Interview topics range from Don and Billie Anne's background, how they teamed up to create Prista's innovative product, ActionCue Clinical Intelligence, what makes ActionCue CI different, and how hospitals and facilities have benefitted through their 11 years in business.
CIHQ is a membership-based organization comprised primarily of acute care and critical access hospitals whose mission is to create a regulatory environment that enables healthcare organizations to effectively deliver safe, quality patient care. CIHQ is a CMS-Approved Accrediting Organization.
Prista is proud to be a CIHQ Partner.
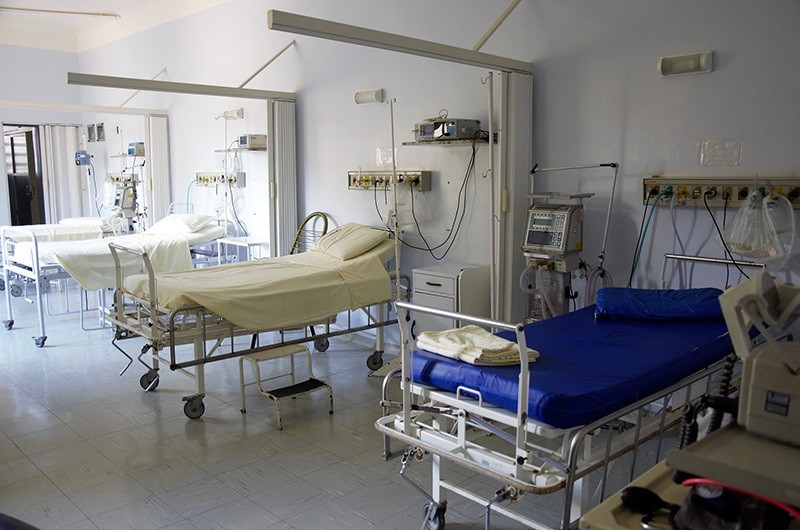
Rural communities in the United States are facing dangerous changes in the healthcare available to them. The financial realities for full-service hospitals with a relatively small number of beds in small communities mean that enormous trade-offs will be made, just to ensure that the hospital in some form can survive.
According to the InDepth article “Rural Hospitals Look for Help To Survive” by Alex Kacik in Modern Healthcare, “The gulf between rural hospitals’ available beds and daily admissions widens every year, causing providers to scale down. Without help from the government or larger health systems, many more will likely close.”
As with organizations of all kinds – when facing financial pressures, ongoing lack of profitability and an inability to attract and retain talent, the search for solutions becomes all-important. Some rural hospitals are forming cooperative purchasing groups, hospital management organizations are finding ways to consolidate and prioritize the services offered, or reducing the number of hospital beds available.
The article continues, “Inevitably, rural communities will have to shutter hospital wings or otherwise pare down, said Lyndean Brick, president of the consultancy Advis Group.”
Yet, with all of these ongoing financial pressures, rural hospitals are still an incredibly critical part of the community ecosystem without which, it is possible that the loss of life and lack of access to healthcare would significantly degrade the quality of life for our small, rural communities.
“These independent hospitals need to find some way to gain scale and leverage to offset margin compression and achieve parity with everyone else who is consolidating around them,” Brenner said.
At the same time rural hospitals work on scaling their patient flow, increasing the effectiveness and efficiency of key process is a critical factor in improving both top-line and bottom-line finances. Technology can certainly play a role in positively impacting rural healthcare organizations in a way that enables them to provide quality care in a cost-effective way. For instance, telemedicine services may create opportunities for specialist consultations without long-distance travel.
As rural healthcare providers take on the challenge of diving more deeply into identifying and addressing the specific needs of their communities, an ability to derive real-time insight into the performance, and facilitate improvement of their organization, will be invaluable. The point to be communicated here is that all hospital have been addressing quality and safety reporting for decades, but now the critical imperatives are to (1) extend the goal from generation and delivery of reports to achieving real clinical performance improvement, and (2) address that goal far more efficiently than has been done in the past. Quality-safety applications like Prista’s ActionCue Clinical Intelligence enable insight and implementation of performance improvement plans that both impact reimbursement and increase care quality.
But let’s be clear. It is not simply the application of some technology that brings about more effectiveness and efficiency, but how that information technology is designed and the goals driving that design. Any software that merely captures basic information about safety events, requiring humans to then organize a PI action plan, go back to the setting of an event to ask questions, gather and process data into a usable and informative format and do numerous other manual and ad hoc administrative functions is not at all improving the efficiency of the overall process. Not until fundamental innovation in IT and process are undertaken, those tools that are simply “reporting” oriented are replaced by a functional platform that truly facilitates the performance improvement process, and saves its users significant time in that pursuit, will progress be made toward the triple aim. That is the only way clinical performance has can be optimized for better operational, regulatory and financial outcomes.
This advice is from Prista’s partner and advisor for HIPAA Compliance, Third Rock. Considering the vast number of individuals impacted by this breach event, and the seriousness of the issue, we thought it would be good to share this. Please consider these steps for your own effort. You can also see this article from their current newsletter, find other resources and subscribe to their newsletter here.
If you would like more insight or help with your organization’s HIPAA Privacy and Security compliance, you can direct any questions or follow-up to Robert Felps at Third Rock, via email or call 512-310-0020.
Stealing headlines from Hurricane Irma was the revelation that Equifax experienced a major data breach during the summer. Equifax is one of the “big three” credit monitoring services and therefore the data they collect on each of us is broad and deep. They estimate that data for 143 million people – nearly half the population of the United States – has been stolen!
What does this breach mean for you? Your financial history and ability to buy a home, new car, or even get healthcare could be at stake. Here are recommended steps to protect you and your family.
- Be skeptical! Equifax is looking out for itself, not you! They will fight to survive this fiasco, spending the minimum required. Don’t give away your rights – read all documents carefully before signing. Don’t rush to sign any agreements. The aftermath of the breach will play out over months, not hours, and new information will emerge every week.
- Be cautious! This breach is so large, scammers will take advantage of it. Be wary of offers to sign up for credit monitoring services and giving out any additional personal information! Validate the authenticity of any such services. Research these services because many do not provide the protection you need or believe you will receive.
- Assume your data has been stolen, even if Equifax says your data has not been stolen! Breaches tend to grow over time because companies often under-report to minimize the bad publicity. As the company investigates the breach, they are also likely to uncover more theft that wasn’t obvious at the beginning of the investigation. For instance, on Tuesday of this week, it was publicized that EquiFax suffered additional breaches this year before this major breach.
- Check the Equifax website set up to inform people if their data was stolen. The link to the site is equifaxsecurity2017.com. Questions abound about whether the website provides accurate responses or not! Remember, be skeptical!
- Keep all your records! Record all your interactions with Equifax. Ask for email confirmations after phone conversations. Save email as PDFs. Any costs you incur, get receipts and put them in a specific location or folder.
- Check your credit report at; https://www.annualcreditreport.com/index.action. This is a free service and you can get one free report a year from each credit reporting service. I recommend getting one report every 4 months from a different service so you can maintain a fairly regular status of your credit information.
- Freeze your Credit – this is your last option and prevents companies from checking your credit score in an effort to get additional credit. This is not something you should do without evaluating your circumstances. If you are planning to purchase a new car, take out a loan, or get a new credit card, you should evaluate your options.




